Stand up for the facts!
Our only agenda is to publish the truth so you can be an informed participant in democracy.
We need your help.
I would like to contribute
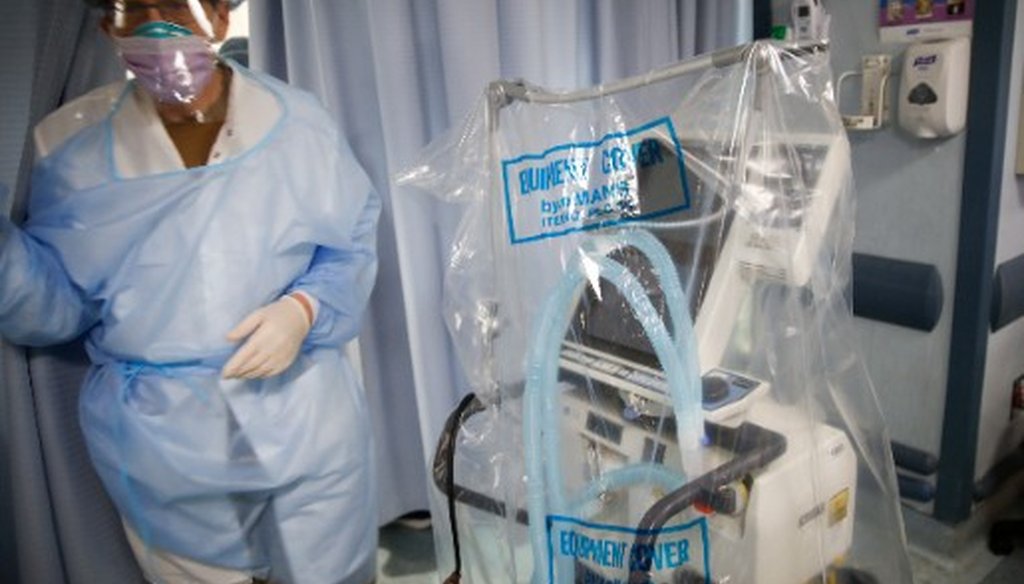
A ventilator waits to be used by a COVID-19 patient going into cardiac arrest, on April 20, 2020, at St. Joseph's Hospital in Yonkers, N.Y. (AP)
If Your Time is short
• A recent study was widely reported to have found an 88% death rate for coronavirus patients who were put on a ventilator, leaving the impression that patients should do everything they can to stay off ventilators. But medical experts say that’s a misinterpretation.
• The 88% death rate was among patients who either died or recovered. It did not account for the roughly three-quarters of patients involved in the study who were still on a ventilator at the end of the study, leaving in doubt what the eventual mortality rate will be.
• A subsequent study finds much lower mortality rates for ventilator patients.
Even within the whirlwind of coronavirus news, a recent study quickly garnered headlines when it reported a high mortality rate for patients on ventilators in one New York health care network.
The study, published in the prestigious Journal of the American Medical Association, followed 5,700 coronavirus patients who had been admitted to 12 Northwell Health hospitals in metropolitan New York between March 1 and April 4.
The finding that painted the grimmest picture, and attracted the most media attention, was about the likelihood that patients put on ventilators would die. Ventilators are medical devices that help patients with compromised lung function continue to breathe. Patients are connected to the ventilator through a breathing tube inserted into the airway, a procedure known as intubation.
The study found that only 38 ventilator patients recovered and were released, compared with 282 who died. That works out to a death rate of 88%.
Glossed over in some of the initial media coverage and often ignored entirely in social media posts was that another 831 patients remained in the hospital and were excluded from the calculation. That’s more than 72% of all the patients involved in the study, so for the vast majority of patients studied, the jury is still out on whether they will recover. (The paper will be updated when outcomes are known for the full group of patients, said Karina Davidson, senior vice president of research at Northwell Health.)
While some media outlets changed their headlines after the authors of the study clarified some of the data, intensive-care specialists bristled at the impression that the widely shared 88% mortality rate finding was making on the public.
Focusing on the 88% number, they said, could lead people to conclude that it’s safer to avoid being connected to a ventilator. But that’s wrong, said Richard H. Savel, an adult-critical-care specialist and a professor of clinical medicine at SUNY Downstate College of Medicine in New York.
No patient would want to become sick enough to be put on a ventilator, but if they do, a ventilator may be the best hope for recovery.
"It’s a misconception that avoiding intubation at all costs will somehow save lives," Savel said.
Key caveats to the study
Another nuance that wasn’t captured in the public discussion is that patients with serious pre-existing conditions, such as heart failure, emphysema or cancer, may face special difficulties recovering from the virus. They may be taken off a ventilator relatively early and be shifted to palliative care or hospice. Because of the short time window of this study, these sorts of patients may be over-represented among those counted in the 88% figure, said Todd W. Rice, an associate professor in Vanderbilt University’s division of allergy, pulmonary and critical-care medicine.
By contrast, the patients who have fewer serious underlying conditions "have the best overall prognosis," Rice said. Those patients are likely to be kept on the ventilator longer, so they may be over-represented in the group whose outcomes are still unknown.
"Mortality statistics, when evaluated so soon during the course of illness, are not helpful," said Colin R. Cooke, an assistant professor in the department of internal medicine at the University of Michigan. "Ideally, we’d like to see what patient outcomes are at 30 to 90 days after onset to get a closer approximation of mortality."
Another factor is that the study was conducted in New York City, the nation’s hardest-hit region for coronavirus, so it may not be representative of the nation as a whole, said Luciano B. Lemos-Filho, an intensive care physician at National Jewish Health in Denver.
A new study, which hasn’t gone through peer review yet, has been posted by researchers at Emory University. It looked at 217 critically ill coronavirus patients at facilities in Georgia, which hasn’t been hit as hard as New York City. It found a far lower mortality rate for patients on ventilators: 29.7%.
"A major factor in mortality seems to be health system stress, meaning how many patients they are managing in the system on a given day and how far above normal that number is," said Greg S. Martin, a professor of medicine at Emory and one of the co-authors of the recent paper.
Michael Gropper, a professor and chair of anesthesia at the University of California-San Francisco School of Medicine, said an ICU environment is especially dependent on calibrated teamwork between nurses, therapists, physicians, and others. A large influx of patients can make that balance difficult to maintain.
How much lower might the mortality rate be?
As more studies are done, researchers will get a better handle on how much overall mortality rates for ventilator patients vary across the country. But experts said they expect the figure to settle well below 88%.
Specialists point to past studies of Acute Respiratory Distress Syndrome, or ARDS, which existed before coronavirus but which can play a key role in severe coronavirus cases.
For instance, a 2016 paper in the Journal of the American Medical Association reported a mortality rate of 34.9% for patients with mild cases of ARDS, 40.3% for those with moderate cases, and 46.1% for those with severe ARDS.
Potentially, COVID mortality rates could end up on the higher end of the spectrum, given the complexity of the disease and how little is understood about its course so far, experts said
Even so, "once we know what the final outcome" for the patients still in the hospital, in all likelihood "the mortality rate will drop significantly," said Ariel L. Shiloh, an associate professor of medicine and neurology at Montefiore Medical Center in the Bronx, New York.
Meanwhile, an improved understanding of the disease’s possible progression is making ventilators an important tool going forward, experts said.
There’s growing evidence that some COVID-19 cases can become serious when the patient has a low level of oxygen but doesn’t realize it.
Low oxygen levels caused by the coronavirus "will cause distress and organ damage," said Michelle N. Gong, a professor at the Albert Einstein College of Medicine who specializes in critical care and epidemiology. "At that point, the ventilator is life-saving."
Our Sources
Safiya Richardson, Jamie S. Hirsch, and Mangala Narasimhan, et al., "Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area," (Journal of the American Medical Association), April 22, 2020
Sara Auld, Mark Caridi-Scheible, James M. Blum, et al., "ICU and ventilator mortality among critically ill adults with COVID-19," April 26, 2020
Washington Post, "In New York’s largest hospital system, many coronavirus patients on ventilators didn’t make it," April 26, 2020
CNN, "About a quarter of Covid-19 patients put on ventilators in New York's largest health system died, study finds," April 26, 2020
Bloomberg, "New Study Shows Nearly 9 in 10 Covid-19 Patients on Ventilators Don’t Make It," April 22, 2020
ABC News, "'Silent Hypoxics': Docs warn of coronavirus link to mysterious low oxygen symptoms," April 28, 2020
The Dispatch, "Have Nearly 90 Percent of Intubated Coronavirus Patients in New York Died?" April 27, 2020
Email interview with Richard H. Savel, adult critical care specialist in Brooklyn and professor of clinical medicine at SUNY Downstate College of Medicine, April 27, 2020
Email interview with Todd W. Rice, associate professor of medicine in Vanderbilt University’s division of allergy, pulmonary, and critical care medicine, April 27, 2020
Email interview with Robert P. Dickson, an assistant professor at the University of Michigan's medical school, April 27, 2020
Email interview with Colin R. Cooke, assistant professor in the department of internal medicine at the University of Michigan's medical school, April 28, 2020
Email interview with Greg S. Martin, professor of medicine at Emory University, April 28, 2020
Email interview with Ariel L Shiloh, associate professor of medicine and neurology at Montefiore Medical Center, April 27, 2020
Email interview with Michelle N. Gong, professor at the Albert Einstein College of Medicine, April 27, 2020
Interview with Luciano B. Lemos-Filho, intensive care physician at National Jewish Health in Denver, April 27, 2020
Interview with Michael Gropper, professor and chair of anesthesia at the University of California-San Francisco School of Medicine, April 28, 2020
Email interview with Karina Davidson, senior vice president of research at Northwell Health, April 28, 2020
































