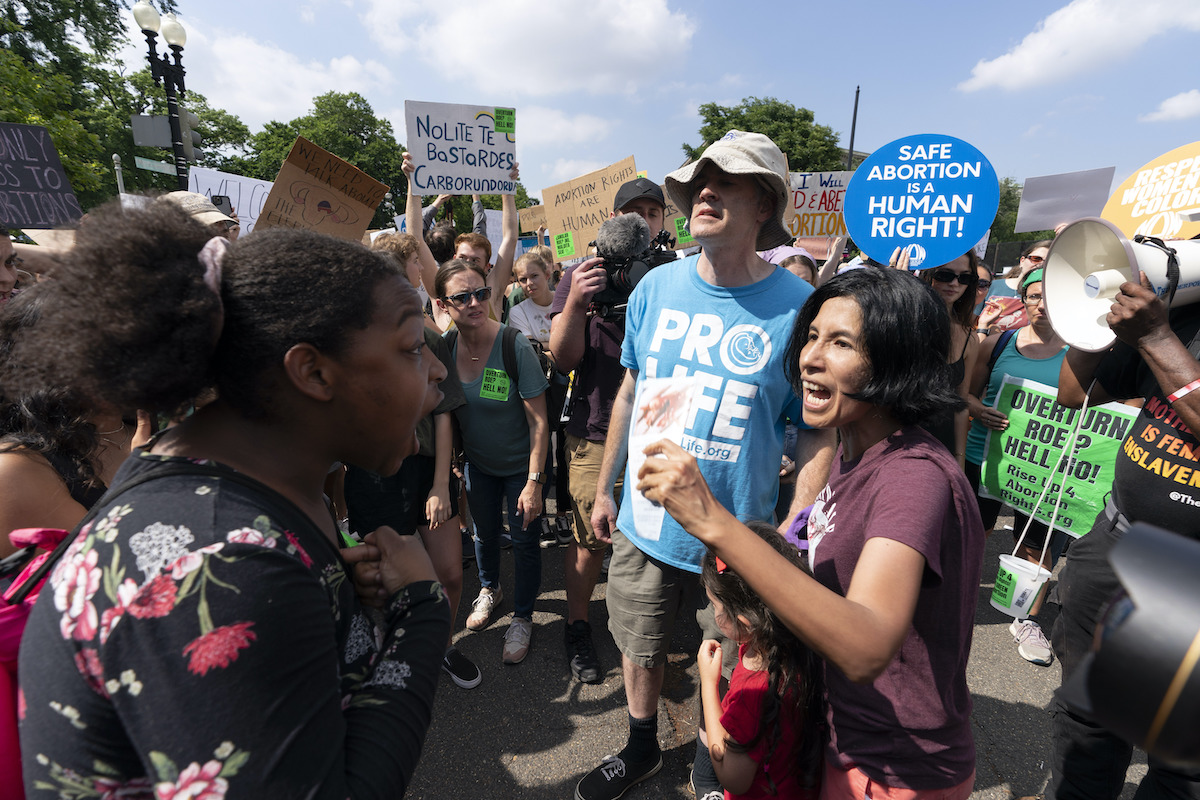Stand up for the facts!
Our only agenda is to publish the truth so you can be an informed participant in democracy.
We need your help.
I would like to contribute
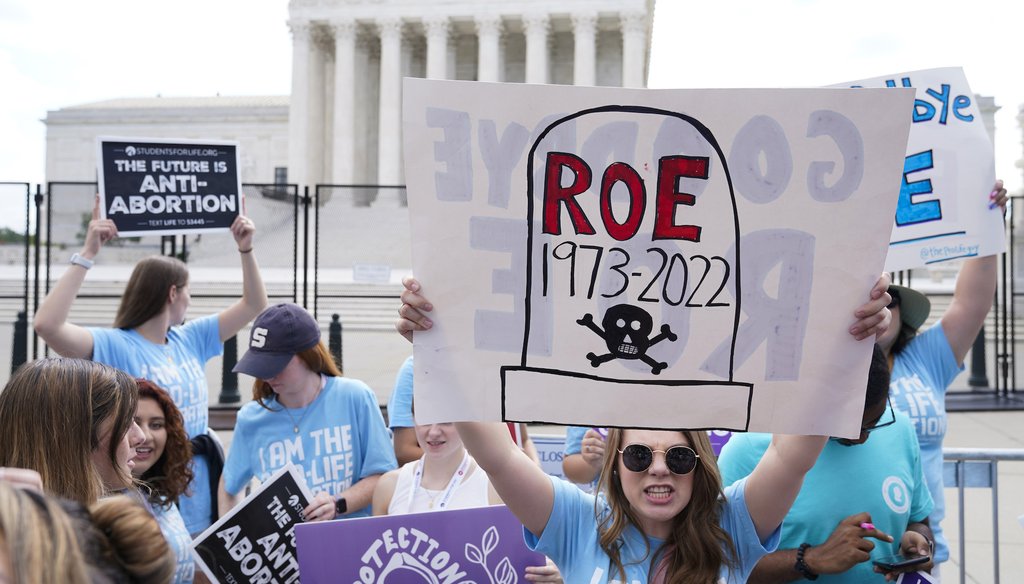
Demonstrators protest about abortion outside the Supreme Court in Washington on June 24, 2022. (AP Photo/Jacquelyn Martin)
Does abortion cause infertility? Can fetuses feel pain in the first term? Is it common for women to seek abortions later in pregnancy?
Google any of these questions and you’ll find a range of contradictory answers.
After nearly five decades of federally protected abortion access in the U.S., the Supreme Court’s June 24, 2022, decision to strike down Roe v. Wade refueled a host of unfounded claims.
Although views diverge on the morality of legal abortion access, research provides real data that can answer some of these questions.
Here, we compiled the most prevalent fact-checkable claims about abortion, along with a few newer claims that have surfaced since Roe was overturned.
Claim: "Abortion is dangerous."
Decades of research has shown that both in-clinic and medication abortions are safe for patients who seek them.
The majority of abortions are performed in outpatient, nonhospital settings, and complications are rare: About 2% of women experience a complication associated with the abortion, according to the American College of Obstetricians and Gynecologists. When complications do occur, most are minor and easily treatable with follow-up procedures or antibiotics.
The risk that a woman will die in childbirth is significantly higher than the risk she will die from an abortion, evidence shows. Serious complications from abortions continue to be rare at all gestational ages.
"One thing people fail to understand is that pregnancy actually carries real risk, and we tend to hide all of the difficult realities about it," said Tracy Weitz, an American University professor and senior fellow with the Women's Initiative at the Center for American Progress, a liberal-leaning think tank.
A 2004 study published in the American Journal of Obstetrics and Gynecology showed that the risk of abortion complications increases as a pregnancy progresses. But researchers say that about 90% of abortions occur within the first trimester, when the procedure is safest.
Medication abortion, a two-drug combination that can be taken up to around 11 weeks into a pregnancy, is considered the most common way to terminate a pregnancy in the U.S., according to data by the Guttmacher Institute, an abortion rights research organization.
Research has shown that patients can safely self-manage their abortions using medication they access through the mail or by telemedicine. But other abortion-inducing methods that some patients turn to, such as intentionally hurting themselves or taking toxic herbs, are inherently dangerous and not recommended.
Claim: "Abortion can cause infertility."
Having an abortion does not typically affect a woman’s ability to get pregnant again.
A 2018 report from the National Academies of Sciences, Engineering, and Medicine on the safety and quality of abortion care found no association between abortion and secondary infertility, the inability to conceive or carry a baby to term after previously giving birth. It also found no association between an abortion and subsequent preterm birth.
Other studies have reaffirmed this and the American College of Obstetricians and Gynecologists maintains abortion does not increase infertility risk.
One rare exception can occur in instances in which uterine scarring results from an infection following a surgical abortion procedure, known as dilation and curettage, or a D and C. This condition is known as Asherman syndrome, which can cause recurrent miscarriages or difficulties conceiving.
But this uncommon condition is not unique to people who get abortions. Patients can also undergo D and C procedures following incomplete miscarriages and in cases in which they deliver a baby but fail to deliver all or part of a placenta. The risk of developing Asherman’s syndrome can also increase if someone has had an operative hysteroscopy, a history of pelvic infections or has been treated for cancer.
Claim: "First-term fetuses can feel pain."
When a person is injured, a signal travels through a series of nerves to the spinal cord and the brain. The information is then transmitted through a web of neurons to the cerebral cortex. It's in this part of the brain that a person perceives the feeling of pain.
The vast majority of research has found that the connections needed to transfer these signals, and the brain structures needed to process them, are undeveloped before 24 weeks of gestation, according to the American College of Obstetricians and Gynecologists. Because a fetus at this stage of development lacks these connections and structures, reproductive experts conclude that a first-term fetus does not have the capacity to feel pain.
"Every major medical organization that has examined this issue and peer-reviewed studies on the matter have consistently reached the conclusion that abortion before this point does not result in the perception of pain in a fetus," the organization says on its website.
Some researchers argue that pain is a subjective experience that’s difficult for doctors to measure. Some researchers have suggested that providers consider anesthetic options for the fetus during an abortion, a service that could carry additional costs.
Weitz said the argument often gets used in politics as a pretext to outlaw abortion altogether. "What I think people need to understand is that even the scientists who are saying, ‘Let’s debate the meaning of pain’ aren’t suggesting it as a justification for banning abortion," she said.
Claim: "Most Americans support abortion."
Abortion is a complex topic that is difficult to poll. U.S. abortion surveys indicate that a slight majority of Americans support some form of abortion access, but not outright. Experts told us that results often vary significantly depending on how pollsters frame questions.
"There is ample evidence that many people are ambivalent about the issue or experience significant cross-pressures in formulating an opinion," Scott Keeter, a senior survey adviser to the Pew Research Center, told PolitiFact in May. "These realities make it quite difficult to sum up abortion attitudes in one or two sentences or with one or two questions."
Polls taken before the Supreme Court’s decision to overturn Roe v. Wade showed that a 2-1 majority of Americans didn’t want justices to take that step. But other survey results show the public’s views on abortion neither start nor end there.
For example, one common question asks whether abortion should be legal in all cases, legal in most cases, illegal in most cases or illegal in all cases.
If support for having abortion legal in all cases and legal in most cases is grouped together, the results in four recent surveys range from 59% to 65%. But if you group together the two middle categories — people who want to allow some abortion rights along with people who desire limited access — these results add up to 54% to 60%.
The circumstances surrounding abortions also elicit nuanced survey responses. A 2018 Gallup poll found that people widely support abortion access after rape or incest, and are more willing to support abortion in the first trimester instead of the third.
University of Notre Dame researchers conducted 217 in-depth interviews across six states in 2019, and concluded, "Abortion attitudes are more complex than survey statistics suggest. Survey summaries can be misleading and should be interpreted with caution."
Claim: "Abortion causes breast cancer."
There is no evidence that abortion causes breast cancer. Decades of research has shown no causal link between the two.
In 1997, the New England Journal of Medicine published a Danish study with 1.5 million participants that used information from national registries and found no link between abortion and breast cancer. The American Cancer Society calls this the largest, and likely most reliable, study on the topic.
"There is no association between a history of abortion and breast cancer. This has been clearly disproven," said Dr. Daniel Grossman, an obstetrics, gynecology and reproductive sciences professor at the University of California, San Francisco.
The claim of a link appears to have stemmed from hypotheses that hormonal changes caused by interrupting a pregnancy could increase a woman’s susceptibility to breast cancer. Research has concluded that this isn’t the case. But the premise is based on the real effects of hormones, which change throughout a woman’s life — including during pregnancy — and can influence the chances of developing breast cancer later in life, according to the National Cancer Institute.
In its 2018 report, the National Academies of Sciences, Engineering, and Medicine said many older studies that explored a possible association between breast cancer and abortion were flawed by recall bias and a lack of controls for important factors such as the woman’s age.
This included one 1996 analysis that, according to the Guttmacher Institute, combined results from numerous flawed studies and concluded that abortion elevated the risk of cancer. Rather than relying on medical records, researchers asked women whether they ever had an abortion — but that methodology creates its own bias, experts say.
"Surveys have shown that 60% of people will not disclose if they’ve had an abortion," Weitz said. "When someone has a disease or chronic illness, they’re more likely to recall and include all of their medical history. So, all the people who didn’t have a reason to disclose that they had abortion are more likely not to tell others."
Several other studies published since the Danish study have also concluded that induced abortion is not associated with an increase in breast cancer risk.
Claim: "Plan B is a form of abortion."
No. Plan B is an emergency contraceptive used to prevent pregnancy. It does not cause abortions.
Plan B, also known as the morning-after pill, is known to be effective only before a pregnancy is established, medical experts said, and can be taken within five days after sexual intercourse.
"Emergency contraception can prevent pregnancy after sexual intercourse and is ineffective after implantation," the American College of Obstetrics and Gynecology said. "Studies of high-dose oral contraceptives indicate that hormonal emergency contraception confers no risk to an established pregnancy or harm to a developing embryo."
A representative for Foundation Consumer Healthcare, the company that owns Plan B, previously told PolitiFact that the medication has 1.5 milligrams of levonorgestrel, "the same active ingredient used in many regular oral contraceptives for over 30 years — just at a single, higher dose," and works by temporarily delaying ovulation.
Scientific data shows that Plan B does not prevent or interfere with implantation of a fertilized egg, will not affect a woman’s fertility and cannot induce an abortion, the company said.
Claim: "More access to contraception increases abortion demand."
Data shows this is wrong.
The U.S. Centers for Disease Control and Prevention reports that most unintended pregnancies result from women not using contraception or using it inconsistently or incorrectly. The Brookings Institution in 2012 found that unintended pregnancies account for more than 90% of abortions.
Research shows that improved contraception use has played a large role in reducing unintended pregnancies and subsequently, abortions.
One 2016 analysis by Guttmacher found that a steep drop in abortions from 2008 to 2011 was driven by a decline in unintended pregnancies spurred largely by more and better contraceptive use.
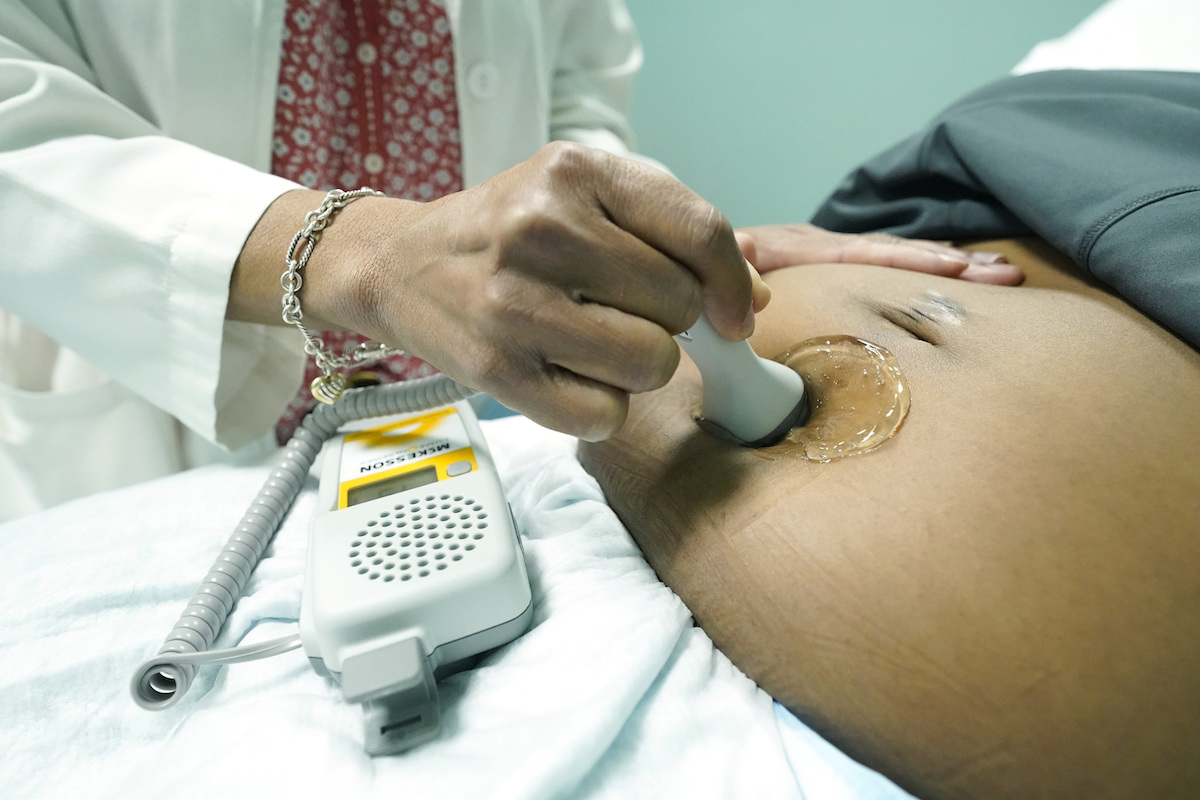
Claim: "A ‘fetal heartbeat’ can be detected at six weeks gestation."
Some states have passed laws to ban abortions around six weeks of gestation, when some anti-abortion advocates say an embryo’s heartbeat is detectable by an ultrasound.
Many medical and reproductive health experts, however, counter that it’s medically inaccurate to describe the sounds heard over an early ultrasound as a heartbeat. Those sounds represent embryonic cardiac activity from a primitive tube of cells, experts said, but the heart is not yet formed and cannot produce an audible heartbeat.
"What is heard is the rhythmic flow of blood through the cardiac tube," Grossman said. "The heart isn’t fully formed until nine to 10 weeks."
Claim: "Women routinely have late-term abortions."
Although we have heard the phrase "late-term abortion" often in political discourse, reproductive health experts say it’s not a recognized medical term.
The American College of Obstetrics and Gynecology says the term has "no medical significance," and is not used in a clinical setting or to describe abortion care later in pregnancy.
"Abortion later in pregnancy is very safe and typically occurs as a result of complications in the life or pregnancy of a pregnant person," a spokesperson for the organization said in an email to PolitiFact. "Approximately 1% to 2% of abortions occur after 21 weeks, and approximately 91% of abortions occur before 13 weeks."
A pregnancy is considered full term from 39 to 40 weeks, and late term at 41 weeks. Anti-abortion activists typically use "late-term abortion" to describe abortions that may happen at 15 or 20 weeks, or even earlier, experts said.
Claim: "The treatment for an ectopic pregnancy is abortion."
Abortion-rights activists have questioned whether Roe v. Wade’s overturning would limit a patient’s ability to receive treatment for an ectopic pregnancy. While ectopic treatment consists of terminating the pregnancy, we found that the process is different from abortion in most cases.
Ectopic pregnancies happen when a fertilized egg implants itself outside of the uterus, usually in one of the fallopian tubes. These pregnancies are not viable and if untreated can lead to life-threatening bleeding. Most of the medical experts we talked to were clear that they don’t consider ectopic treatment an abortion, but they noted that the lack of consensus over how abortion is defined makes defining ectopic pregnancy treatment confusing.
Treatments for ectopic pregnancies depend on how far along the pregnancy is. In most cases, the condition is treated as soon as possible to avoid the fallopian tube from rupturing. If detected early enough, ectopic pregnancies can be treated with a prescribed medication called methotrexate.
The drug can be used alongside another medication, misoprostol, to end viable, first-trimester pregnancies. But the price and possible side effects make it less likely to be used in abortions, Amy Addante, an OB-GYN and fellow with Physicians for Reproductive Health, told PolitiFact.
If an ectopic pregnancy is farther along, or if it leads to the fallopian tube bursting, the patient will need surgery. This can be done laparoscopically; a doctor makes a small incision and uses a thin tube with a camera and light to perform the surgery. If an emergency surgery is required, a doctor will make an incision in the patient’s abdomen.
Neither of these procedures are performed in a surgical abortion.
But reproductive health experts told us that the larger issue is whether medical providers interpret restrictive abortion laws as limiting their ability to treat patients with ectopic pregnancies, which comes down to how abortion is defined.
In medical terms, abortion is broadly considered a procedure undertaken to end a pregnancy. When it comes to legal definition, however, what constitutes an "abortion" is often dictated partly by whether the patient made a conscious decision to terminate.
Our Sources
American College of Obstetricians and Gynecologists, Combating Abortion Myths: The Tool Kit, Accessed Feb. 11, 2023
National Library of Medicine, Incidence of emergency department visits and complications after abortion, Jan. 2015
National Library of Medicine, The comparative safety of legal induced abortion and childbirth in the United States, Feb. 2012
National Library of Medicine, Risk factors for legal induced abortion-related mortality in the United States, April 2004
Guttmacher Institute, Abortion and Mental Health: Myths and Realities, August 2006
Guttmacher Institute, Medication Abortion, Feb. 1, 2021
Action Canada for Sexual Health & Rights, Abortion myths and facts, Accessed Feb. 11, 2023
Planned Parenthood, Facts about Abortion Care, July 27, 2020
Annals of Internal Medicine Journal, Health of Women Who Did and Did Not Terminate Pregnancy After Seeking Abortion Services, Aug. 20, 2019
Journal of Medical Ethics, Reconsidering fetal pain, 2020
Live Science, Do Fetuses Feel Pain? What the Science Says, Aug. 3, 2022
National Academies of Sciences, Engineering, and Medicine, The Safety and Quality of Abortion Care in the United States, 2018
The New England Journal of Medicine, Induced Abortion and the Risk of Breast Cancer, Jan. 9, 1997
Cancer.org, Abortion and Breast Cancer Risk, June 19, 2014
American College of Obstetricians and Gynecologists, Facts Are Important: Identifying and Combating Abortion Myths and Misinformation, Accessed Feb. 17, 2023
American College of Obstetricians and Gynecologists, Facts Are Important: Gestational Development and Capacity for Pain, Accessed Feb. 17, 2023
New York Times, Abortion Opponents Hear a ‘Heartbeat.’ Most Experts Hear Something Else, Feb. 14, 2022
Healthline, Can Abortion Cause Infertility?, Updated Jan. 16, 2020
Cleveland Clinic, Asherman's Syndrome, Accessed Feb. 26, 2023
PolitiFact, Fact-checking the false claim that Plan B causes abortions, June 30, 2022
American College of Obstetricians and Gynecologists, Emergency Contraception, Sept. 2015
PolitiFact, More access to contraception increases abortion demand? No, that’s not right, Jan. 18, 2023
PolitiFact, Why polling about abortion hides the true complexity of what Americans think, May 5, 2022
PolitiFact, What do Americans think about abortion policy? It can be complicated, June 24, 2022
Gallup, Abortion poll, Accessed Feb. 27, 2023
University of Notre Dame, How Americans Understand Abortion, 2020
PolitiFact, How treatment of ectopic pregnancy fits into post-Roe medical care, June 30, 2022
Mayo Clinic, Ectopic pregnancy, March 12, 2022
Email interview, Rachel Kingery spokesperson at the American College of Obstetricians and Gynecologists, Feb. 15-16, 2023
Phone interview, Tracy Weitz, professor at American University and senior fellow with the Women's Initiative at American Progress, Feb. 17, 2023
Email interview, Dr. Daniel Grossman, professor of obstetrics, gynecology and reproductive sciences at the University of California, San Francisco, Feb. 19-20, 2023