Stand up for the facts!
Our only agenda is to publish the truth so you can be an informed participant in democracy.
We need your help.
I would like to contribute
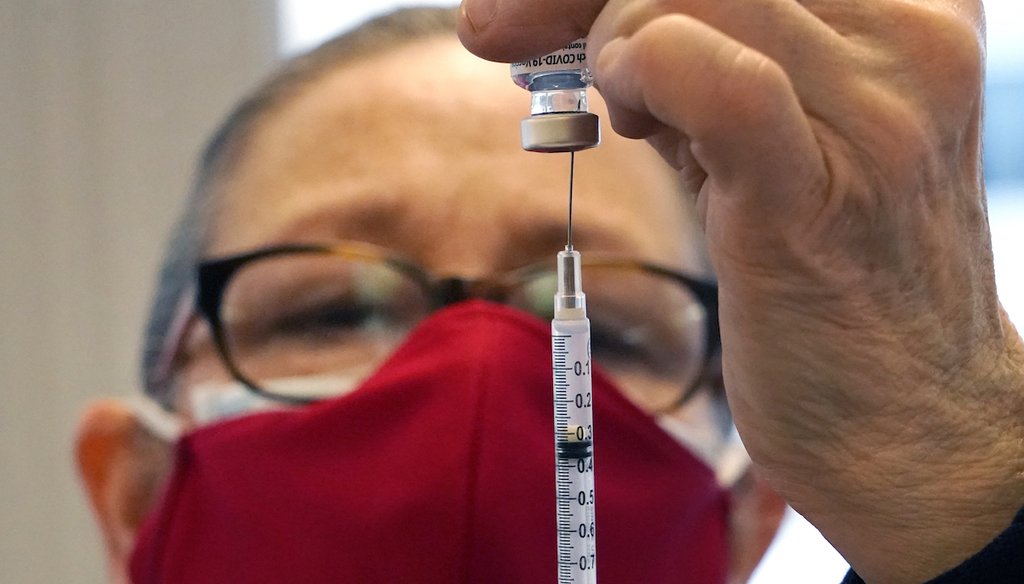
Healthcare volunteer Melissa Lowry prepares a COVID-19 vaccine at a regional vaccination site in Massachusetts. (AP Photo/Elise Amendola)
If Your Time is short
-
Ethnic information is missing for about half of the people vaccinated in the first month of the rollout.
-
Some people can spread the virus even after being vaccinated, and public health researchers say we need to know more about that risk.
-
The U.S. gathers limited information on the virus’ mutations, which would be essential for tracking vaccine effectiveness and responding quickly to new variants.
Right now, vaccine rollout is a numbers game. The nation has a pretty good idea of how many doses have gone to each state and county. The government’s COVID-19 vaccination dashboard shows how many people have received their second shot — over 5.9 million as of the time we wrote this.
Getting shots in arms is Job One, but the broader drive to corral the coronavirus, save lives and get the country back to normal hinges on having data that so far is limited, or in some cases, close to absent.
We asked 12 epidemiologists and public health researchers for the biggest information gaps that they see. Some of their concerns center on communities that have been hit hardest by COVID-19. Some center on the unknown impact the vaccines will have on virus spread. Viruses are tricky organisms, and the return to something close to the old daily routines could well depend on the country being equipped to think two steps ahead.
Targeting high risk areas
During the first month of vaccinations, about 13 million people got at least one dose. For just about all of them, there’s data on their age and sex. But ethnicity information is missing for nearly half, with some experts pointing to inconsistent methods of data collection at the local level.
"We need solid ethno-demographic information on all vaccines to ensure that resources are focused on populations at greatest risk," said Donald Thea, professor of global health at Boston University School of Public Health.
Blacks, American Indian/Alaska Natives and Hispanics, as the latest CDC report noted, have seen the highest rates of illness and death from the virus.
Marcella Nunez-Smith, head of the White House’s COVID-19 equity task force, said during a Feb. 1 press briefing that getting ethnic data into the system is urgent.
"I’m worried about how far behind we are," she said. "We cannot ensure an equitable vaccination program without data to guide us."
Experts said it’s unclear how the addition of dozens of federally run mass vaccination sites could affect rural distribution and state plans. And it remains to be seen how they will better reach people who need the vaccine most, such as communities of color.
"What strategies were used in the initial vaccination outreach?" said Beth Blauer, executive director of Centers for Civic Impact at Johns Hopkins University. "Anecdotally — because we don’t have the data — we are seeing that there are significant disparities on who is getting access to appointments."
Getting back to normal
Vaccines are the right tool to break the chain of transmission, but several of the experts we reached said scientists don’t fully understand how the shots change a vaccinated person’s ability to spread the disease. That ability doesn’t completely go away.
Biostatistician Natalie Dean at the University of Florida said the extent to which vaccines reduce the amount of the virus a person produces, or how long they produce it, is unclear. Asymptomatic individuals have already been shown to be a key driver of the virus’ spread, and vaccination doesn’t totally shut that process down.
A group of Boston University researchers that included Thea, Davidson Hamer and Eleanor Murray underscored the importance of this uncertainty.
"It’s the single most important unanswered question, because without a clear answer to this, we can’t make solid plans for how to bring life back to normal, post-vaccines," Murray said.
Preliminary data from Moderna showed its vaccine reduced asymptomatic transmission by one-third after the first dose. That is welcome news, Hamer said, and he’s eager to see these data himself, "as they would help me to sleep better."
In a new study, the AstraZeneca vaccine, which still needs U.S. approval, reduced overall transmission by two-thirds.
To be sure, vaccinations remain the best bet for preventing infection. But because of the lingering risk of asymptomatic transmission, people who get vaccinated are told to keep wearing a mask.
With the ever-changing landscape of vaccine availability, our panel of experts also said there could be a lot of practical value in knowing what happens to people when their first shot comes from one drugmaker, such as Pfizer, and the second from another, such Moderna. Some initial animal studies suggest protection levels could go up.
Whether antibodies come through a vaccine or by natural exposure, the promise of being able to freely go to a restaurant or have a drink with a friend hinges on knowing more about how well antibodies shut down the virus.
Matthew Laurens, a pediatric infectious-disease specialist at the University of Maryland, said scientists don’t yet know how large an individual’s antibody army needs to be in order to be effective. That’s important for a number of reasons, including predicting how long a vaccination provides protection.
It would also be helpful to know whether catching the virus delivers longer-term immunity from future infections, said Nicole Gatto, an associate professor at Claremont Graduate University’s School of Community and Global Health.
Mutations and avoiding unintended consequences
The virus variants from the United Kingdom, South Africa and Brazil complicate the path ahead. Many of the experts we reached lamented the limited effort in the United States to study the genetic makeup of the variants that pop up.
"How common are the U.K., South African and Brazillian variants?" said Tara C. Smith, a professor of epidemiology at Kent State University's College of Public Health. "What about other homegrown variants? We’re not doing nearly enough sequencing to know right now."
Having that information in hand would shine a light on how well current vaccines work on slightly different versions of the coronavirus. However, in the absence of a quick test to determine which version caused an infection, this can be expensive and time-consuming.
"We’re pretty much blind right now, and the lagging indicator of rapidly rising infection rates, as we shockingly saw in the U.K. and Ireland, becomes evident when it’s too late," Thea said.
Laurens, of the University of Maryland, said that having that genetic data could help drugmakers produce vaccines that work across all variants. Booster shots might still be needed to assure immunity to all strains, he said, but having a cross-section of genetic data would speed the process of creating new vaccines.
There’s another, more urgent, reason to track the viral genotypes. Vaccinations have the potential to spur mutations beyond the ones we are already seeing. Like any other evolutionary force, attacking one form of the virus can lead to new forms that are less vulnerable to the vaccine.
If people skip the second dose of the vaccine, that potentially could boost the opportunity for vaccine resistant strains to develop.
The best way to head that off in the future is to do a lot more genetic sampling today.
RELATED: What we know about the COVID-19 variants and how they impact vaccine efficacy
Our Sources
Centers for Disease Control and Prevention, COVID-19 Vaccine, Feb. 2, 2021
Centers for Disease Control and Prevention, Mortality and Morbidity Weekly Report, Feb. 1, 2021
Health Policy Watch, Vaccines Could Help Reduce Asymptomatic Virus Transmission – Although More Evidence Is Needed, June 1, 2021
University of Oxford, Oxford coronavirus vaccine shows sustained protection of 76% during the 3-month interval until the second dose, Feb. 2, 2021
New York Times, U.S. Pharmacies Will Start to Get a Big Infusion of Vaccines, Feb. 3, 2021
Email interview, Nicole Gatto, associate professor at Claremont Graduate University’s School of Community and Global Health, Feb. 1, 2021
Email interview, Matthew Laurens, pediatric infectious disease specialist at the University of Maryland, Feb. 1, 2021
Email interview, Tara C. Smith, a professor of epidemiology at Kent State University's College of Public Health, Feb. 1, 2021
Email interview, Natlie Dean, biostatistician at the University of Florida, Feb. 1, 2021
Email interview, Dr. Amesh Adalja, senior scholar at the Johns Hopkins University Center for Health Security, Feb. 1, 2021
Email exchange, Donald M. Thea, professor, and associate chair, Department of Global Health, Boston University School of Public Health, Feb. 1, 2021
Email exchange, Davidson Hamer, professor of global health and medicine, Boston University School of Public Health, Feb. 1, 2021
Email exchange, Eleanor Murray, assistant professor of epidemiology, Boston University School of Public Health, Feb. 1, 2021
Email interview, Dr. Seema Yasmin, director of research and education programs at the Stanford Health Communication Initiative, Feb. 1, 2021
Email interview, Beth Blauer, executive director of Centers for Civic Impact at Johns Hopkins University, Feb. 2, 2021
Email interview, William Moss, executive director of the International Vaccine Access Center in the Bloomberg School of Public Health, Feb. 2, 2021
Email interview, Jennifer Nuzzo, senior scholar at the Center for Health Security in the Bloomberg School of Public Health at Johns Hopkins, Feb. 2, 2021












































